|
2/23/2023 0 Comments Define sonogram 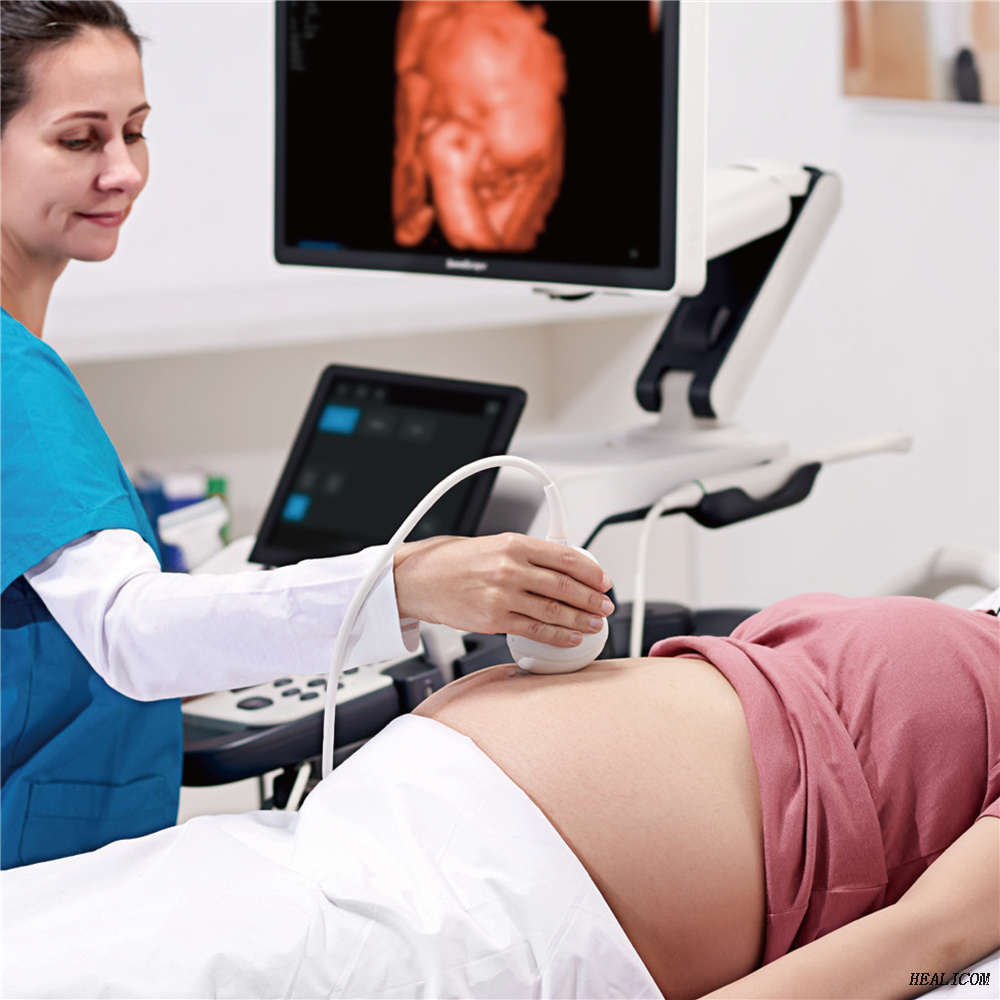
Ultrasound in Obstetrics and GynecologyDiagnostic Ultrasound in Obstetrics: Obstetrics. In the case of a complete placenta previa, a cesarian section is required for delivery to avoid the risk of fetal and maternal hemorrhage. As the fetus grows and the uterus expands, the lower uterine segment thins and grows disproportionately, such that in most cases the placenta is no longer low-lying by a follow-up study (usually performed at 32-34 weeks). 
Treatment and prognosisĪ low-lying placenta is relatively common in the second-trimester morphology scan. Sagittal images best demonstrate the relationship of the placenta to the internal cervical os. MRI is the gold standard imaging modality for the placenta and its relationship to the cervix, although in most instances it is not required. If it lies within a few centimeters of the cervical os, then a repeat ultrasound at ~32 weeks should be performed to ensure that the edge has migrated further away. Sometimes grades I and II are termed a "minor" or "partial" placenta previa, and grades III and IV are termed a "major" placenta previa 5.ĭue to placental trophotropism, the diagnosis of a placenta previa is not usually made before 20 weeks.ĭuring the 'routine' 18 to 21-week morphology scan, the distance between the lower edge of the placenta and the internal os should be measured. grade IV: complete previa: placenta completely covers the internal cervical os.grade III: partial previa: placenta partially covers the internal cervical os.grade II: marginal previa: placental tissue reaches the margin of the internal cervical os, but does not cover it.grade I: low-lying placenta: placenta lies in the lower uterine segment but its lower edge does not abut the internal cervical os (i.e lower edge 0.5-2.0 cm from internal os).Previa is divided into four grades depending on the relationship and distance to the internal cervical os: The term "placenta previa" covers a spectrum of anomalies and results from the partial or total insertion of the placenta into the lower uterine segment. maternal/fetal compromise secondary to exsanguination.Other associated clinical features include: 
Placenta previa usually presents with painless vaginal bleeding in the second half of pregnancy (>20 weeks gestation), most commonly between 34-38 weeks gestation. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
